If you have ever felt a sharp pinch in the front of your hip when squatting, running, or even sitting for long periods, you may have heard the term hip impingement. It is one of the most common diagnoses among active adults, especially those who lift weights, run, or participate in rotational sports.
For many people, being told they have hip impingement can feel confusing or even concerning. Questions like “Is something wrong with my hip structure?” or “Will I need surgery?” are common.
The reality is that hip impingement is often misunderstood. While it can involve structural factors, it is rarely just a structural problem. In many cases, it is more about how the hip is moving, loading, and functioning within the body as a whole.
This article will break down what hip impingement actually is, why it happens, the most common symptoms, and how it can be treated effectively without relying on fear-based or overly simplistic approaches.
What Is Hip Impingement?
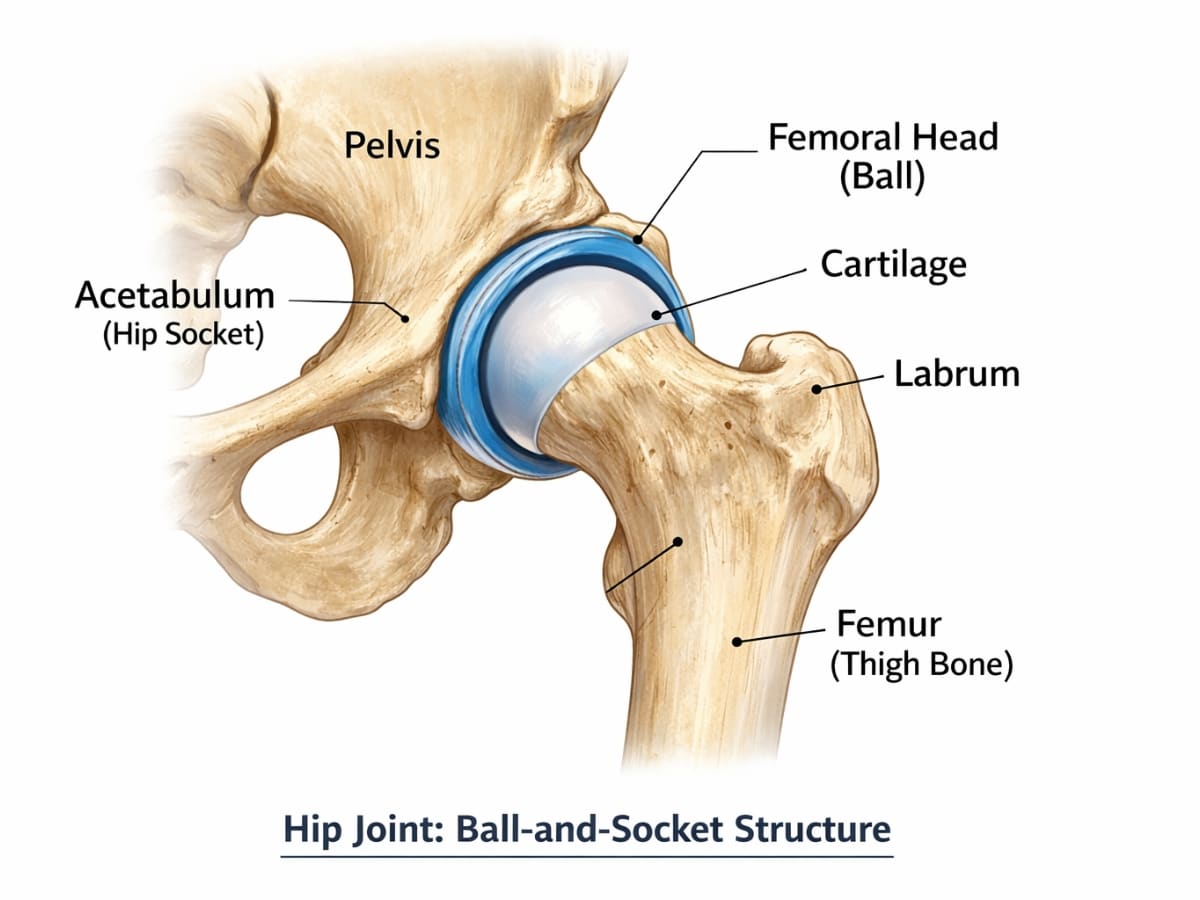
Hip impingement, often referred to as femoroacetabular impingement (FAI), occurs when there is abnormal contact between the ball of the hip (femoral head) and the socket (acetabulum).
This contact can create a pinching sensation, especially during movements that involve deep hip flexion, such as squatting, lunging, or sitting.
There are typically two types of hip impingement:
- Cam impingement: where the ball of the hip is not perfectly round
- Pincer impingement: where the socket covers too much of the ball
Some individuals have one type, while others may have a combination of both.
However, it is important to understand that many people have these structural variations without any pain at all. This is a key point that often gets overlooked. Research has shown that imaging findings consistent with hip impingement are common even in people with no symptoms.
Why Hip Impingement Is So Common in Active Adults
Hip impingement is especially common in people who are active. This includes weightlifters, runners, athletes, and even individuals who spend long periods sitting during the day but train regularly.
There are a few reasons for this.
First, many popular exercises place the hip into deeper ranges of flexion. Squats, lunges, and certain gym movements all require the hip to move through positions where impingement symptoms are more likely to appear.
Second, repetitive movement patterns can lead to adaptations in how the body moves. Over time, the body may lose access to certain ranges of motion while overusing others.
Third, lifestyle factors like prolonged sitting can influence hip positioning and movement. Sitting for long periods often places the hips in a flexed position, which can contribute to stiffness and altered movement patterns.
When these factors combine, the hip may begin to move in a way that increases stress at the front of the joint.
Common Symptoms of Hip Impingement
Hip impingement can present in a variety of ways, but there are some common patterns that many people experience.
The most typical symptom is a pinching or catching sensation in the front of the hip. This is often felt during movements like:
- Squatting or lunging
- Sitting for long periods
- Getting up from a chair
- Running or sprinting
Other symptoms may include:
- Deep hip stiffness or tightness
- Reduced range of motion
- Clicking or catching sensations
- Pain that may radiate into the groin or upper thigh
In some cases, symptoms may come and go depending on activity levels.
Why Hip Impingement Is Not Just a Structural Problem
One of the biggest misconceptions about hip impingement is that it is purely a structural issue.
While structural variations can play a role, they do not automatically cause pain.
Research has shown that many people with cam or pincer morphology have no symptoms at all. This suggests that structure alone does not determine whether someone experiences pain. Systematic reviews have found that these imaging findings are actually quite common in people without any hip pain.
Instead, symptoms are often influenced by how the hip is moving and how load is being distributed through the joint.
If the body lacks mobility, control, or coordination, certain areas of the joint may experience more stress than others. Over time, this can lead to irritation and discomfort.
The Role of Movement Patterns in Hip Impingement
Movement patterns play a major role in how hip impingement develops and persists.
If the hip is consistently positioned in a way that limits space within the joint, the likelihood of experiencing pinching or discomfort increases.
For example, if the pelvis is positioned forward and the lower back is extended, the hip joint may be placed into a position where the front of the joint is more compressed.
Similarly, if the body favors one side more than the other, asymmetrical loading patterns can develop. These patterns may cause certain tissues to take on more stress over time.
Addressing these underlying movement tendencies is often a key part of long-term improvement.
Why Rest, Stretching, or Generic Exercises Often Don’t Work
Many people try to manage hip impingement by resting, stretching, or performing general strengthening exercises.
While these strategies can provide temporary relief, they often fail to create lasting change.
Rest may reduce irritation, but it does not address the underlying movement patterns. Stretching may improve flexibility, but it does not necessarily improve how the joint is controlled during movement.
Generic strengthening exercises can help build capacity, but if they are not aligned with the individual’s movement needs, they may reinforce existing compensations.
This is why symptoms often return once activity levels increase again.
What Effective Treatment for Hip Impingement Looks Like
Effective treatment for hip impingement focuses on improving how the hip functions within the entire system, not just addressing the local area.
This typically involves several key components.
Restoring Movement Options
The first step is often improving the ability of the hip to move through different positions. This may include targeted exercises that address limitations in rotation, flexion, or extension.
Improving Strength and Control
Once movement improves, the next step is building strength within those ranges. This helps the body control movement more effectively and distribute load more evenly.
Addressing Whole-Body Coordination
The hip does not function in isolation. The trunk, pelvis, and surrounding joints all influence how the hip moves. Treatment often includes exercises that improve coordination across these areas.

Gradual Return to Activity
As symptoms improve, activity levels are gradually increased. This helps the body adapt to higher levels of stress without triggering flare-ups.
The goal is not just to reduce pain, but to build resilience.
When Does Imaging Matter?
Imaging such as MRI or X-ray can provide information about the structure of the hip, but it should be interpreted carefully.
Findings like cam or pincer morphology are common and do not always correlate with symptoms.
In many cases, treatment decisions should be based more on how the individual moves and functions rather than imaging alone.
This approach helps avoid unnecessary fear and allows for more effective, individualized care.
Long-Term Outlook for Hip Impingement
The outlook for hip impingement is generally positive when addressed appropriately.
Many people are able to return to their preferred activities without pain by improving movement patterns, building strength, and managing load effectively.
The key is moving away from the idea that the hip is “damaged” and instead focusing on how it can function better.
With the right approach, the hip can become more adaptable and resilient over time.
Moving Forward With Confidence
Hip impingement can feel limiting, especially for active individuals who want to train, compete, and move freely.
But understanding what hip impingement actually is, and what it is not, can change how you approach it.
Rather than viewing it as a fixed structural problem, it can be seen as a movement issue that can be improved.
When treatment focuses on restoring movement, building strength, and addressing the system as a whole, lasting improvement becomes possible.
And for many people, that shift is the difference between managing symptoms and getting back to doing what they enjoy.



